Abstract
Introduction: The chronic kidney disease (CKD) is an irreversal progressive process which takes to a terminal state, where patients need permanent dialysis or even a transplant. It has been shown that the lung function and ventilatory capacity are compromised in these patients, increasing the alteration with exposure to hemodialysis and sedentarism.
Objective: To compare the lung function and ventilatory capacity of hemodialysis patients, according to exposure to intradialysis physical training.
Material and Methods: Study of quantitive type, not experimental, descriptive and transverse. The study population included 12 ambulatory patients between 40 and 80 years old, undergoing hemodialysis with arteriovenous fistula in the dialysis unit of Valdivia’s Central Hospital, and who obtained more than 24 points in the Minimental Test. The statistical analysis was performed with the SPSS program (version 11.5 for Windows) and the level of statistical significance through the Wilcoxon and Mann-Whitney test (p<0.05).
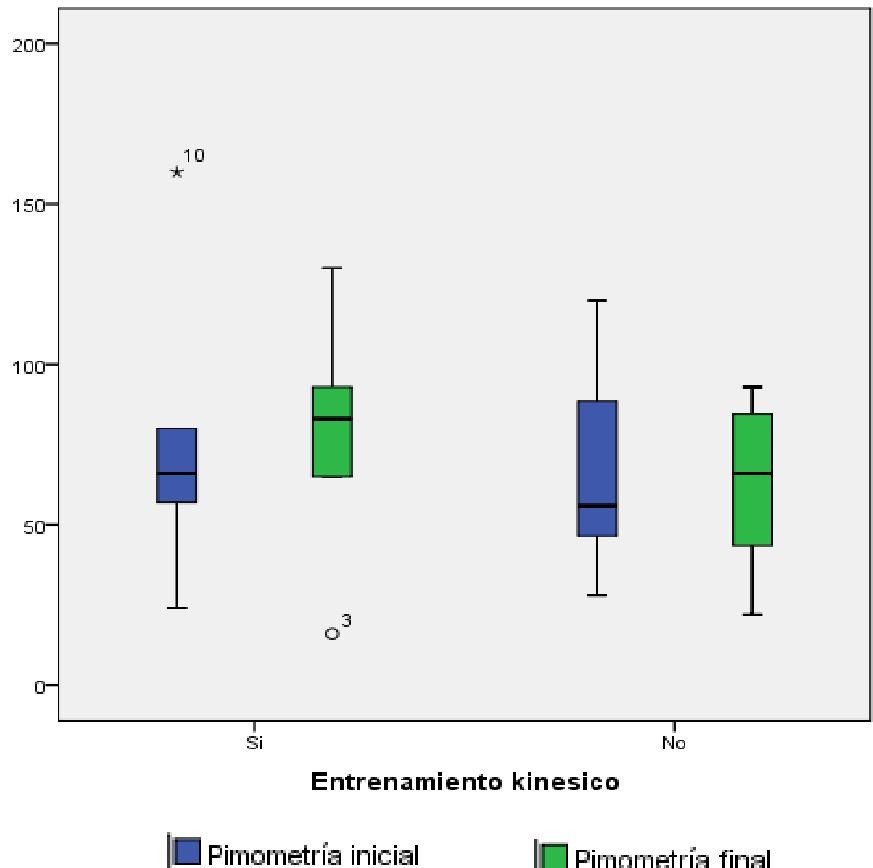
Results: The comparison of the initial and final pimometry in patients with and without physical training did not show a statistically significant difference (p>0.05), however it was observed that the subjects exposed to physical training have higher values in the initial and final maximum inspiratory pressure compared to those who have not been trained.
Conclusion: Intradialysis physical training causes a positive effect on the respiratory system. The subjects submitted to hemodialysis tend to present under predicted values in both lung function and ventilatory capacity, being mostly affected with aging and time of exposure to hemodialysis.
References
Gorostidi M, Santamaría R, Alcázar R, Fernández-Fresnedo G, Galcerán JM, Goicoechea M, et al. Documento de la Sociedad Española de Nefrología sobre las guías KDIGO para la evaluación y el tratamiento de la enfermedad renal crónica. Nefrología 2014; 34(3):302-16. Available from: https://doi.org/10.3265/Nefrologia.pre2014.Feb.12464
Couser WG, Remuzzi G, Mendis S, Tonelli M. The contribution of chronic kidney disease to the global burden of major noncommunicable diseases. Kidney International 2011;80. Available from: https://doi.org/10.1038/ki.2011.368
Kidney Disease Improving Global Outcomes (KDIGO). Clinical Practice Guideline on the Management of Diabetes and Chronic Kidney Disease. [Internet] 2018 [Accedido el 01/07/2019] Disponible en: https://kdigo.org/wp-content/uploads/2018/03/ KDIGO-DM-GL-SoW-Public-Review-FINAL.pdf
Sociedad Chilena de Nefrología. Registro de diálisis XXXVIII Cuenta de Hemodiálisis Crónica (HDC) en Chile (al 31 de agosto de 2018) [Internet]. Valparaíso: Sociedad Chilena de Nefrología; 2018 [citado 01 de julio 2019]. Disponible en: https://www.nefro.cl/v2/biblio/registro/24.pdf
Mukai H, Ming P, Lindholm B, Heimbürger O, Barany P, Stenvinkel P, et al. Lung Dysfunction and Mortality in Patients with Chronic Kidney Disease. Kidney Blood Press Res 2018;43:522-535.. Available from: https://doi.org/10.1159/000488699
Artom M, Moss-Morris R, Caskey F, Chilcot J. Fatigue in advance kidney disease. Kidney International 2014;86:497-505. Available from: https://doi.org/10.1038/ki.2014.86
Bahey H, Salam F, Takey K. Effects of inspiratory muscle training on pulmonary functions and muscle strength in sedentary hemodialysis patients. J Phys Ther Sci 2018;30:424-7. Available from: https://doi.org/10.1589/jpts.30.424
De Souza R, Fernandes N, Moraes J, De Moura M, De Moura M, Do Valle B, et al. Pulmonary function and exercise tolerance are related to disease severity in pre -dialytic patients with chronic kidney disease: a cross-sectional study. BMC Nephrol. 2013;14:184-92. Available from: https://doi.org/10.1186/1471-2369-14-184.
Pu J, Jiang Z, Wu W, et al. Efficacy and safety of intradialytic exercise in haemodialysis patients: a systematic review and meta-analysis. BMJ Open 2019;9:e020633. Available from: https://doi.org/10.1136/bmjopen-2017-020633
Gutiérrez M, Beroíza M, Borzone G, Caviedes I, Céspedes J, Moreno R, et al. Espirometría: Manual de procedimientos SER Chile. Rev Chil Enferm Respir 2018;34:171-188. Available from: https://doi.org/10.4067/S0717-73482018000300171
Black L, Hyatt R. Maximal respiratory pressures normal values and relationship to age and sex. Am Rev Respir Dis. 1969;99:696-702.
Costa D, Gonçalves H, Peraro de Lima L, Ike D, Cancelliero K, Montebelo M, I. New reference values for maximal respiratory pressures in the Brazilian population. J Bras Pneumol.2010;36:306-12. DOI: Available from: https://doi.org/10.1590/s1806-37132010000300007.
Safa J, Noshad H, Ansarin K, Nikzad A, Saleh P, Ranjbar A. Effect of Hemodialysis on Pulmonary Function Tests and Plasma Endothelin Levels. Saudi J Kidney Dis Transpl 2014; 25(4):781-7. Available from: https://doi.org/10.4103/1319-2442.135003
Rojas M, Dennis R. Valores de referencia para parámetros de espirometría en la población adulta residente en Bogotá. Biomédica. 2010;30:82-94. Available from: https://doi.org/10.7705/biomedica.v30i1.156
LoMauro A, Aliverti A. Sex differences in respiratory function.Breathe 2018;14:131-40. Available from: https://doi.org/10.1183/20734735.000318
Yilmaz S, Yildirim Y, Yilmaz Z, Veysel A, Mahsuk K, Melike T, et al. Pulmonary Function in Patients with End Stage Renal Disease: Effects of Hemodialysis and Fluid Overload. Med Sci Monit. 2016;22:2779-84. Available from: https://doi.org/10.12659/MSM.897480
Sharma A, Sharma Ash, Gahlot S, Prasher P. A study of pulmonary function in end-stage renal disease patients on hemodialysis: a cross-sectional study. Sao Paulo Med J. 2017;135(6):568-72. Available from: https://doi.org/10.1590/1516-3180.2017.0179150817
Palamidas A, Gennimata S, Karakontaki F, Kaltsakas G,1 Papantoniou I, Koutsoukou A, et al. Impact of Hemodialysis on Dyspnea and Lung Function in End Stage Kidney Disease Patients. BioMed Research International 2014;ID 212751:1-10. Available from: https://doi.org/10.1155/2014/212751
Tavana S, Hashemian S, Jahromi F. Effect of Dialysis on Maximum Inspiratory and Expiratory Pressures in End Stage Renal Disease Patients. Tanaffos 2015;14(2):128-33. Available from: https://doi.org/10.1371/journal.pone.0173159
Karacan O, Tutal E, Uyar M, Eyübo?lu FO, Sezer S, Ozdemir FN. Pulmonary function in uremic patients on long-term hemodialysis. Ren Fail. 2004;26:273-8. Available from: https://doi.org/10.1081/JDI-120039526
Rocha C, Araújo S. Evaluation of maximum respiratory pressures in chronic renal patients at the pre and post hemodialysis moment. J Bras Nefrol. 2010;32(1):105-11. Available from: https://doi.org/10.1590/S0101-28002010000100017
Silva VG, Amaral C, Monteiro MB, Nascimento DM, Boschetti JR. Effects of inspiratory muscle training in hemodialysis patients. J Bras Nefrol. 2011 Mar;33:62-8. Available from: https://doi.org/10.1590/S0101-28002011000100009
De Souza V, De Oliveira D, Mansur M, Da Silva N, Gomes M. Sarcopenia in chronic kidney disease. J Bras Nefrol 2015; 37(1):98-105. Available from: https://doi.org/10.5935/0101-2800.20150014.
Fatima SS, Rehman R, Saifullah, Khan Y. Physical activity and its effect on forced expiratory volume. J Pak Med Assoc. 2013 Mar;63:310-2.
Adamopoulos S, Schmid JP, Dendale P, Poerschke D, Hansen D, Dritsas A. Combined aerobic/inspiratory muscle training vs. aerobic training in patients with chronic heart failure. European Journal of Heart Failure 2014;16(5):574-82. Available from: https://doi.org/10.1002/ejhf.70